It is often suggested that one must not rely on employer-provided health insurance. Hence, nowadays many of us have multiple health insurance policies. However, we hardly know of how the claim process works and whom to approach in case of multiple health insurance policies.
Before proceeding further, let us understand why we try to buy multiple health insurance policies. There are many reasons and few of them are as below.
- Inadequate existing coverage
- Higher premiums of the existing plan
- Bad claim experience with the insurer
- Multiple plans as backup to avoid risk of claim rejection
- Different kinds of health plans to cater to different health contingencies
- Long waiting periods, etc.
Now let us understand few terminologies which are used in case of general insurance.
# Fixed or Defined benefit plans
Usually, products like critical illness or accidental insurance are considered as fixed benefit plans. Let us say, you have critical illness cover of Rs.10 lakh. Once the insured diagnosed with the critical illness , then irrespective of the cost of expenses of hospitalization insurance company will pay you Rs.10 lakh. Here the identification of disease mentioned in policy is important. Based on the other conditions, insurance company pay the full sum insured amount. The insurance company will not bother about the cost of such critical illness. Same applies to accidental insurance also.
# Indemnity benefit plans
Health insurance will be considered as indemnity benefit plan. Because the claim amount payable from health insurance company is based on the ACTUAL cost but not on the sum assured you opted. Let us say, you have health insurance of Rs.10 lakh and hospitalization cost is Rs.4 lakh, then health insurance company will not pay you Rs.10 lakh, but only Rs.4 lakh (subject to conditions).
# Principle of Contribution
If a policyholder buys insurance plans from different health insurance providers to cover a specified health event. In the event of a claim, then the insurer reserves the right to seek the proportionate amount of claim from the other insurers as well basis this principle.
It is like you buy Rs.5 lakh each health insurance cover from 4 health insurance companies. So you will have a total cover of Rs.20 lakh. In the case of claim of Rs. 6 lakh, then the insurance companies will share this claim amount proportionately among all. The single insurance company or 2-3 insurance company will not be allowed to settle the claim.
However, after the changes in IRDA regulation 2013, there are some changes to this contribution clause. Let see what IRDA Health Insurance Regulation, 2013 says ”
- If two or more policies are taken by an insured during a period from one or more insurers, the contribution clause shall not be applicable where the cover / benefit offered:
- is fixed in nature;
- does not have any relation to the treatment costs;
- In case of multiple policies which provide fixed benefits, on the occurrence of the insured event in accordance with the terms and conditions of the policies, the insurer shall make the claim payments independent of payments received under other similar policies.
- If two or more policies are taken by an insured during a period from one or more insurers to indemnify treatment costs, the insurer shall not apply the contribution clause, but the policyholder shall have the right to require a settlement of his claim in terms of any of his policies
a. In all such cases the insurer who has issued the chosen policy shall be obliged to settle the claim without insisting on the contribution clause as long as the claim is within the limits of and according to the terms of the chosen policy
b. If the amount to be claimed exceeds the sum insured under a single policy after considering the deductibles or co-pay, the policyholder shall have the right to choose insurers by whom the claim to be settled. In such cases, the insurer may settle the claim with contribution clause.
c. Except in benefit policies, in cases where an insured has policies from more than one insurer to cover the same risk on indemnity basis, the insured shall only be indemnified the hospitalization costs in accordance with terms and conditions of the policy”
I will sum up the whole thing. If you have fixed or defined benefit plans, then the contribution clause will not come into the picture. This I already explained above.
-If you have fixed or defined benefit plans, then the contribution clause will not come into the picture. This I already explained above.
-If you have indemnity plans, then based on the cases the contribution clause can be invoked.
What are the cases where such contribution clause can be invoked?
Let us try to understand this whole funda with few examples.
Case 1– Here Mr. Ajay possesses two critical illness health insurance policies with company A coverage of Rs.10 lakh and company B coverage of Rs.25 lakh. Then what will happen in the case of he diagnosed with a critical illness? 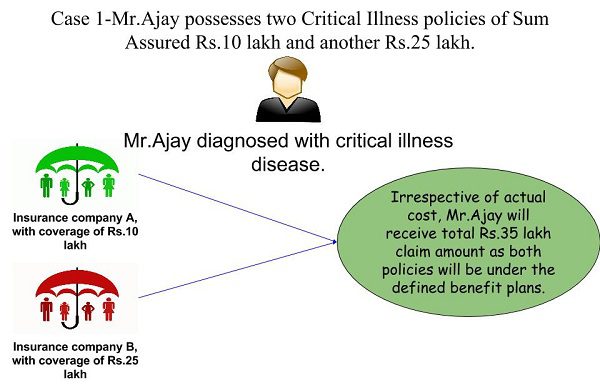
You notice, that critical illness or accidental insurance policies will come under defined or fixed benefit plans, both companies obliged to pay the FULL SUM ASSURED (subject to post fulfillment of the terms and conditions of the plan). Once the claim amount paid, then policy seizes there itself.
Case 2-Here Mr. Ajay possesses one health insurance plan of Rs.5 lakh from company A and one accidental insurance plan of Rs.25 lakh from company B. He met with an accident and the hospitalization cost was Rs.4 lakh. Then how much amount he will receive?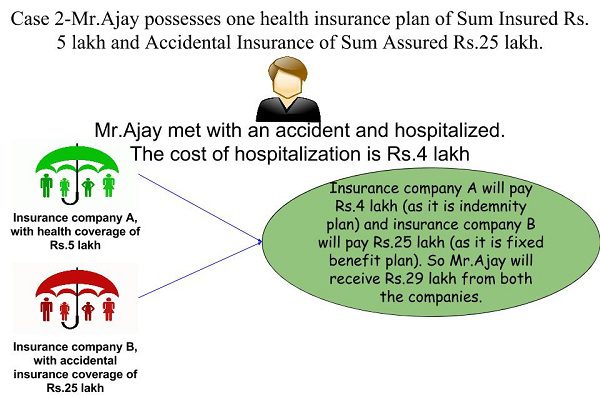
You noticed that insurance company A paid the actual cost of hospitalization. However, insurance company B pays the full sum assured irrespective of the actual cost (subject to the conditions explained in policy document).
Case 3-Here Mr. Ajay possesses two health insurance policies of Rs.5 lakh from insurance company A and Rs.4 lakh from insurance company B. Here two possibilities are there and try to explain both.
Possibility A-Mr.Ajay hospitalized and the bill amount is Rs.3 lakh. Note that this Rs.3 lakh is less than the health insurance coverage provided by both insurance companies. In such situation, he can approach either insurance company A or insurance company B. It is purely his wish. His claim will be accepted by any one company he approaches. I explained the same in below image.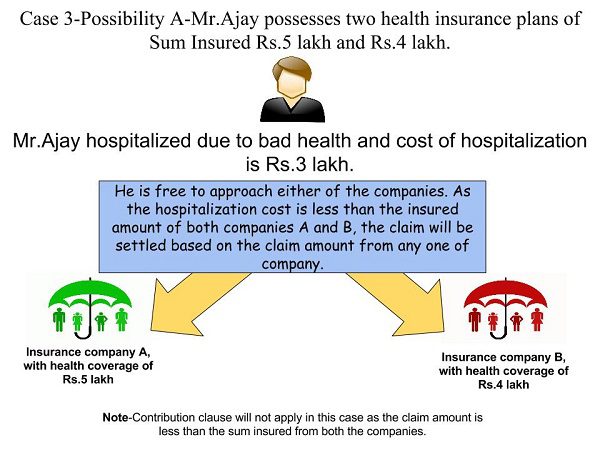
Possibility B-Mr.Ajay hospitalized and the bill amount is Rs.4.5 lakh. Note that this Rs.4.5 lakh is less than the health insurance coverage provided by insurance company A. But it is more than the health insurance coverage provided by B.
In such a situation, if he approaches the insurance company A, then the contribution clause will not apply. Insurance company A will settle the amount (subject to condition) easily as the claim amount is less than the sum insured under the plan.
If he approaches the insurance company B, then the contribution clause will come into the picture. The insurance company will accept the claim amount of Rs.2 lakh (Rs.4,00,000*Rs.4,50,000/Rs.9,00,000). Remaining Rs.2,50,000 will be payable by insurance company A (Rs.5,00,000*Rs.4,50,000/Rs.9,00,000).
I explained the above scenario in below image. 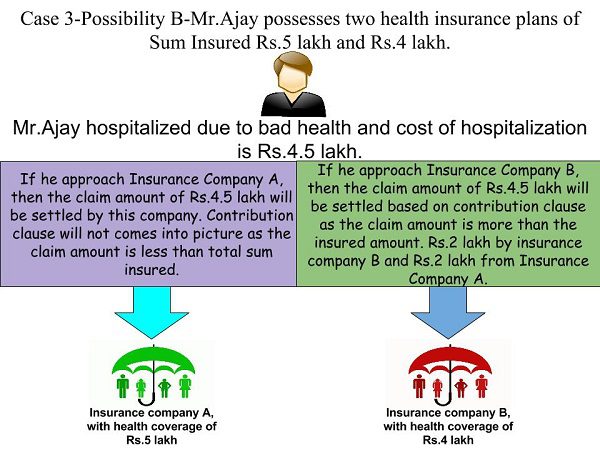
Possibility C-Mr.Ajay hospitalized and the bill amount is Rs.6 lakh. Note that this Rs.6 lakh is more than the health insurance coverage provided by both the insurance companies A & B. So in this case, at any cost the health insurance companies will insist for contribution clause. The claim will be settled as below.
Rs.3,33,333 will be settled by insurance company A (Rs.5,00,000*Rs.6,00,000/Rs.9,00,000). Rs.2,66,666 will be settled by insurance company B (Rs.4,00,000*Rs.6,00,000/Rs.9,00,000). I tried to expalin the same from below post. I explained the same from below iamge.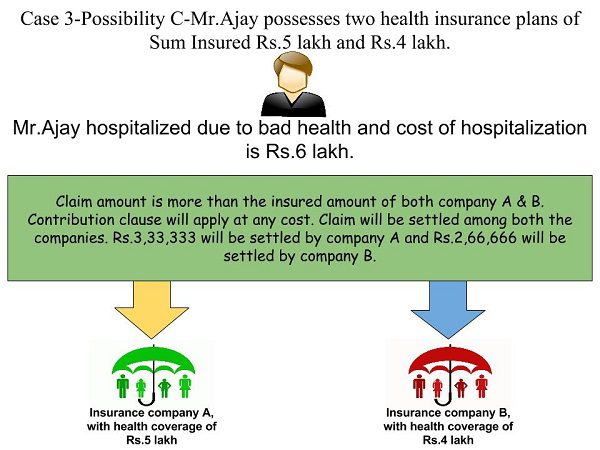
Hope all scenarios are now clear. Let us now discuss the claim process in case of single policy and multiple policies
It is imperative to inform all the insurers about the event.
# In case of Reimbursement:
Collect all the requisite documents from the Hospital and submit the required ones to the respective insurer you are filing the claim from.
- Duly filled Claim Form
- Medical Certificate confirming the diagnosis of the kind of Critical Illness
- Discharge Summary
- Investigation Reports
- Other supporting documents to prove the illness, etc.
(Requirements and documents may vary from insurer to insurer)
# In case of Cashless Treatment:
The chosen insurer or insurers will settle the claim directly with the hospital as per the limits of the health plans and later the contribution clause may be exercised, or you may follow the claims process of the respective insurer from whom you want to claim the balance amount as per the claim specifications.
Other factors to be considered while filing a claim with multiple insurers
- Claims efficiency of the insurers
- Claim settlement turn around time of the insurers
- List of network hospitals of the insurers
- Claim formalities of the insurer
- Efficiency of associated TPA of the insurer
- Previous Claim experience with the insurers
- Check on No claim Bonus status
- Assess the sub-limits and other related clauses in your respective policies
- Claim from your Group Health Policy first
Few points to note regarding having multiple health insurance products-
- You are not allowed to be in profit in case of health insurance policies. The claim amount will be settled based on the actual cost. Because such plans are indemnity plans.
- It will not make sense to have multiple insurance products in think that one company reject means another company may accept it. It is very rare.
- In some cases having multiple health insurance products is beneficial. For example, if you bought a health insurance long back before you diagnosed diabetic then you bought one more plan where the diabetic disease is in waiting period condition, then claim due to diabetic may be claimed by the first insurance.
- It is always best to first claim your company provided health insurance. Because there loading due to claim or some other issues will not pop up. Because it is group insurance and claim settlement will be easy.
- When you are buying multiple health insurance products, then always inform the subsequent insurance companies about your existing cover.
- Always keep in mind that buying one big sum insured plan is cheaper than having multiple health insurance products. Hence, always try to buy big sum insured single product. If in future you need further insurance, then you can use the top up or super top up options.







40 Responses
Will contribution apply if I have primary floater policy of 7.5 lacs and another company’s super top up policy of 25 lacs with 5 lacs as deductible. If my expenses are 10 lacs, then,
1. will the expenditure between 5 to 7.5 lacs be shared by both companies ???
2. will the primary insurer will pay online 5 lacs saying that 5 to 7.5 lacs will be shared on prorata basis?
OR
3. will the primary insurer settle the claim of 7.5 lacs ans the balance 2.5 lacs can be claimed through top up policy???
please clarify
Dear Nitin,
1) Your base plan will pay only up to Rs.7.5 lakh and remaining by super top up.
Another scenario:
I have two insurance policies of 5 lacs and 4 lacs respectively and the cost of treatment exceeds the sum of both, i.e., 9 lacs. I have claimed cashless of Rs 5 lacs from my first insurer. Can I claim another 4 lacs as cashless from my second insurer?
Dear Pratha,
Yes.
Hi,
My Company is reimbursing Medical expenditure incurred upto 75%, I have also a Medical Insurance of Rs. 3,00,000. I incurred an amount of 1,90,000 for OPD (Rs. 30,000) and IPD (Rs. 1,60,000).
I claimed from Insurance co Rs. 1,60,000 and receive a settlement of Rs. 90,000 after deducting limits and co-payment.
Now i claimed my share of Expenditure i.e. Rs. 1,00,000 ( 30,000 +70,000) form my company with remaining original bills, copy of bills submitted to Ins. co and Claim settlement report.
But Company Refuses Rs. 70,000 as i already claimed it in Insurance company and i dont have original bill.
My query is :
1. Can i claim amount of my expenditure from both places i.e. remaining part Rs. 1,00,000 from my company?
2. What document i need to furnish
3. It is allowed ? As you mentioned by Referring IRDA regulation 2013, Please mention where it is written.
Thanks
Dear Rohit,
You are not allowed to claim the same expenses at two places. Also, yes producing original bills is mandatory.
Than you Sir for your quick reply.
However, i would like to discuss it further.
please have a look CGHS rule by following link https://cghs.gov.in/showfile.php?lid=5116
it will show a pdf.
texts are :”MRC claimed from dual source (CGHS and Medical Insurance Company)
In case the beneficiary is also covered under Insurance and the claim has been settled by the
Insurance Agency, the liability of CGHS will be reimbursement to the extent of balance of
total claim after payment by insurance company subject to the maximum amount of CGHS
rate”
If i am not wrong you can claim your remaining part from your company’s medical insurance company as per IRDAI clarifications issued on 10th January 2017 in respect of provisions of IRDA(Health Insurance) regulations 2016 guidelines .
IRDAI clarification Letter Ref. no. IRDA/HLT/REG/CIR/005/01/2017
Dear Amit,
He can claim the remaining amount from other insurance if he has. But he can’t claim the same claim from multiple insurer for the same amount.
Hi Basavaraj!
So in this case Rohit’s remaining claim of Rs 100000/-(IPD – 70000 + OPD – 30000) can be claimed from his company’s insurer ?
Because his personal insurer cleared only Rs 90000/- out of the total IPD claim of Rs 160000/- (Remaining IPD – 70000).
IRDAI clearly states in clarification Letter (Ref. no. IRDA/HLT/REG/CIR/005/01/2017) that “policy holder having multiple policies shall also have the right to prefer claims from other policy/policies for the amounts disallowed under the earlier chosen policy/policies, even if the sum insured is not exhausted.”
Thought of discussing this case for my better understanding. Your inputs/guidance will be highly appreciated. Thanks
Dear Amit,
Yes, can claim but do remember that the company insurance will also have the approximately the same limit on IPD claim. In that case, as his own insurance accepted it, they may deny the claim. Buying multiple insurances does not mean getting 100% claim to be settled by applying with all the insurers.
Hi,
Me and my my wife both are having insurance from our respective corporate. Both corporate have different insurance company but same TPA.
I have my my wife as well in my coverage.
Me and my wife both have same maternity cover, Rs 50K (normal delivery) and 75 K (Surgery delivery).
Say if the maternity package of the hospital is more than the capped amount of insurance company, then the total amount can be claimed using the “Contribution Clause”?
While filling the form for Cashless facility at hospital, will providing the details of policies of us both will do required?
Say if the expense of the delivery comes to 1 Lac, then both the insurance company will contribute accordingly and we do not have to worry about the cap of 50K in our policies?
Please clarify the doubts on the same.
Thanks in Advance.
Rishi- This is what I have already explained in above post. Please read once again.
My DOB is 24/05/1952. I am having an Individual policy from National Insurance for 5 lakhs which covers my pre existing diseases BP and DVT. I had DVT in 2000 and had operation. I do take medicine for the control of BP and DVT. I do not have any other problems. I am 90 kg weight and 167 cms of height with about BMI of 30.I am having the policy from national Insurance from the last 23 years. Now I wanted to get super top up policy as additional protection for 10 lakhs with deductable 5 lakhs. I approached united India they rejected because 60 years is the limit for any approval from their under writers. I approached HDGC Ergo they rejected my proposal because my BMI. Does any company will provide me super top up policy and not top up with the above circumstances. Does DVT,BMI and BP as pre-existing disease will lead to complete rejection for new policy like super top up by any company in India ? If so is there any way to get a policy ? Pl advice.Thanks .
Subramanya-It is hard to get at such age and with such health complication. I can’t surely say which company offers you. But you try your luck.
Hi
I was admitted to breach candy hospital for ACUTE EMBOLIC STROKE WITH ATRIAL FIBRILLATION ICU Breach Candy Hospital I have two covers one of Rs Three Lacs under group cover of my Bank and personal from New India Assurance of Rs.Four Lacs now bill amt was ONE Lac Eighty Six Thousand and cash less from my Bank amt received Ninty Five Thousand for the remaining incremental cost i submitted claim papers in time to NEW INDIA who rejected claim. Please guide.
Diplaxmi-What reason they quoted?
Very nice article. It would be more better if you highlight on super top up plan. So, I hv a query whether cashless from my base policy & top up policy simultaneously approve by 2 different TPA if base SI is exhausted on Interim bill amount.
Shrenik-Simultaneously is possible only when you submit two set of original bills to both insurers. Is it possible? I already written about super top up plan. Refer here “Top Up Health Insurance Plan & Super Top Health Insurance Plan-What are they?“.
i have decided to take new india health insurance. my question is that if i apply through online portal rather then to purchase through their AGENT My Yearly premium is lesser if go with online or is same
DD-In my view YES or NO (in case of health insurance). But check first online then approach an agent.
Mr. Basavaraj,
Great article. This year I was planning to buy additional health insurance other than company provided but could not as I was not sure about claims procedure in case of multiple insurances. Your article explained it very clearly.
One question – My company provided family cover is from United India. Can I buy personal additional family insurance from same provider i.e. United India? I have selected United India based on your article only (http://www.basunivesh.com/2016/01/26/best-health-insurance-company-india-based-irda-2014-15-incurred-ratio/). Also, it will be easier in claim settlement in case of contribution clause comes into picture.
Thanks
Nitin
Nitin-Yes, you can go ahead.
Hi,
I am 24 employed in BOI and looking for a personal accident insurance plan. I have zeroed in on some plans but before proceding further I would like to clarify a few points.
1- During the policy period, suppose I met with an road accident, say a car rammed my bike (:-)) and fortunately a didn’t die and is hospitalised then will the insurace company took care of my hospitalization expenses incurred for things like surgery, medicines, room charge, etc. (of course subject to sum assured)
2- If yes in Pt. 1 above then will there be any category cap on such expenses like a limit of, say, 100000 on meds, 10k on docs consultation, etc etc.
3- Can you please suggest/refer some good PA plans to me.
Mayur-1) Yes, but with certain conditions. 2) Yes. 3) Refer my post “Best Accidental Insurance Policy in India-How to choose them?“.
Nice article.Thanks for sharing information.
Thanks for the valuable information.
I understand that, the insurance company would ask for the original bills and related documents for claim settlement. So how can we provided the original documents to two different companies?
Shubh-Good question. Either you can take the bill photocopies and get it attested by hospital or you can take the declaration from the first insurer that the details of the bills submitted by an insured.
Dear Basu,
Great write up ! When started reading nothing went in the head, specially IRDA clauses. But amazing illustration and clear explanations . Hats off to you Sir!!
Saleem-Pleasure 🙂
Sir,
Thanks for the informative info on multiple health insurance.The old health insurance policy has very low room rent charges which are not justified in today’s time for example total coverage is Rs 250000 per year and you opt for the room for single bed where room rent is around Rs 7000/day.As per policy you are entiled for 1% of your insured sum that is 2500/day.
now as you have opted for single room of Rs 7000/day, the charges for all facilities is increased by 35 to 50 %,which insurance company refuses to pay.The policy holder has to pay himself the difference of bill at the time of discharge.
Will this difference amount can be claimed from my second insurance?
Indra-NO, you can’t claim that difference amount.
Sir,
Thanks for your nice post.I have a question to ask:
If an insurance company declines your claim on filmsy ground & takes too long to decide about denial(say about one year),is it possible to claim the same amount from other insurance company citing the reason for delay i.e denial by other company.
Rahul-Usually there is a time limit to claim for your hospitalization. It is like 10, 20 or 30 days from the hospitalization or discharge from hospital. If you fail to submit the claim within this day, then no insurer accept the claim. It is the fault of the insurance company which is delaying the claim.
very useful information article
Dear Basavaraj Tonagatti,
Very Useful and explained in such a simple and effective manner . It is extremely important for all of us to understand how to make a claim for medical expenses from Health Insurance companies and most find it complicated and complex process.
Thank you so much for this article Sir
Varun Shah
Varun-Pleasure 🙂
Dear Sir,
It was very informative article and very rarely addressed. I had not come across such topic.
I have few questions..
1) Is it possible to continue employer provided insurance by any chance after retirement from the Company?.
I am sure it is not possible but felt there might be some clauses
2) In case of multiple insurance, which policy should be given preference in case any claim arises- Company provided or bought on our own if Claim amt expected to be within sum insured of both policies.
3) I have recently taken additional coverage to take care of post retirement period, since existing company provided cover will be discontinued after retirement and taking fresh policy may be not be possible due to health issues or heavy premium amount due to higher age. I am 56 yrs old and will be retiring at 60
Thanks once again and all the best wishes!
Rajendra-1) NO. Because it is group insurance.
2) Better for company provided. Because NCB will continue to benefit from the one you owned.
3) That’s good idea.
nice